Introduction
In October 2020, the Departments of Health and Human Services, Labor, and Treasury (collectively referred to as the “Departments”) released the Transparency in Coverage Final Rules (TIC) requiring, among other things, that non-grandfathered health plans disclose, on a public website, three machine-readable files disclosing health care rates. On December 27, 2020, the Consolidated Appropriations Act (CAA) was signed into law. The CAA included extensive transparency reforms, including some that appeared to overlap with TIC rules, but with more aggressive deadlines.
On August 20, 2021, CMS issued guidance that will defer enforcement of some of the CAA provisions, and clarified the relationship between TIC and CAA requirements.
Following is a brief description of the recent guidance as it affects Western Growers Assurance Trust health plans.
Machine Readable Files
The TIC requires non-grandfathered health plans to disclose, on a public website, three machine-readable files showing (i) in-network provider rates for covered items and services, (ii) out-of-network allowed amounts and billed charges for covered items and services, and (iii) negotiated rates and historical net prices for covered prescription drugs. The requirement is effective for plan years beginning on or after January 1, 2022.
The August 20 CMS guidance indicates that two exceptions would be made to the enforcement of the TIC’s machine-readable file requirement:
1. Prescription Drug File. Enforcement related to the prescription drug pricing file will be deferred while the Departments consider, through notice-and-comment rulemaking, whether the prescription drug machine-readable file requirement remains appropriate.
2. In-network and Out-of-Network Files. Given the number of CAA provisions effective on January 1, 2022 and the time and effort required to make the machine-readable files available by the same date, the Departments will defer enforcement until July 1, 2022 of the requirement to make in-network rates and out-of-network allowed amounts and billed charges available on machine-readable files. For plan years beginning on or after July 1, 2022, plans should post the machine-readable files in the month in which the plan year begins.
Self-Service Tool
The TIC and CAA created overlapping requirements for price comparison tools, with different effective dates. The TIC requires plans to make price comparison information available through a web-based self-service tool and in paper form upon request for 500 items and services, for plan years beginning on or after January 1, 2023. The CAA requires similar disclosures, but allow participants to also receive the information over the telephone. The CAA requirements were to be implemented for plan years beginning on or after January 1, 2022.
The Departments intend to propose rulemaking to align the TIC and CAA requirements, and will defer enforcement of the CAA’s January 1, 2022 implementation date to plan years beginning on or after January 1, 2023.
Advanced Explanation of Benefits
The Departments acknowledge that compliance with the advance EOB requirements is likely not possible by January 1, 2022, and intend to undertake notice and comment rulemaking in the future to implement the provision. Until that time, the Departments will defer enforcement of the requirement that plans and issuers must provide an Advanced EOB.
Reporting Requirements for Pharmacy Benefits and Drug Costs
Enforcement of the requirement to report specified information will be delayed. Plans are strongly encouraged to start working to ensure that they are in a position to be able to begin reporting the required information with respect to 2020 and 2021 data by December 27, 2022.
Summary
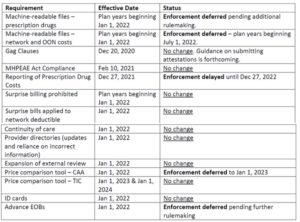
Following is a chart showing the major provisions of TIC and CAA, along with the current enforcement status as described in “FAQs About Affordable Care Act and Consolidated Appropriations Act, 2021 Implementation Part 49,” available on the HHS website.